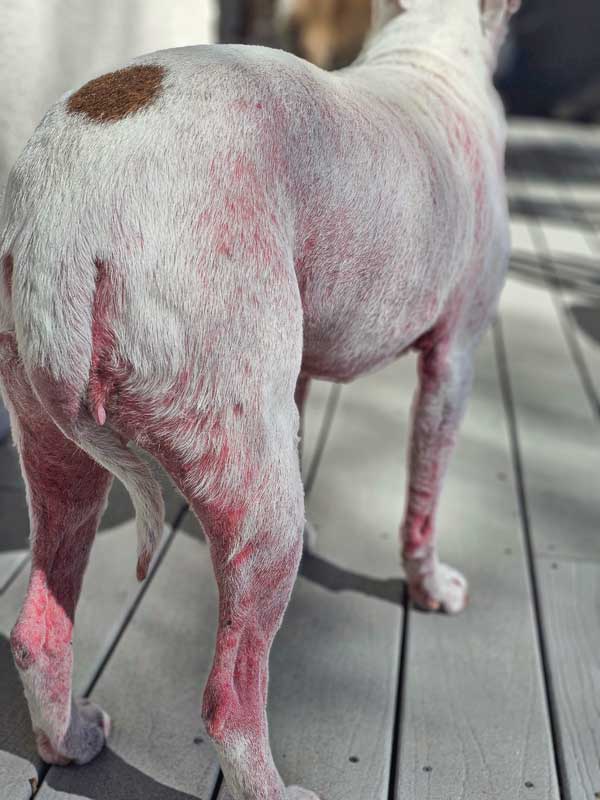
allergies, food allergies, and a resistant bacterial infection. Improvement in this case
was not noted until all three factors were identified and managed. Photo courtesy Dr. Rebecca Mount
Allergic dermatoses are chronic, often lifelong, pruritic skin conditions that can dramatically impact the quality of life of the pet and disrupt the human-animal bond. Additionally, since allergies are incurable and there is a marked variability in clinical presentations, workup and management of allergic diseases can be frustrating for the managing veterinarian.
In allergy cases where it seems nothing is working, returning to the basics and reviewing common complications can help get treatment back on track.
During treatment of allergic diseases, it is common to hit roadblocks that can prevent clinical improvement and increase owner and veterinarian frustrations. These roadblocks include development of secondary infections, uncertain or multiple allergic triggers, ineffective treatment protocols for atopy, and issues with owner compliance. Approaching and overcoming these roadblocks can help improve response to treatment and clinical improvement for the pet.
1) Developing secondary infection
Due to the inflammatory nature of allergic dermatoses, development of concurrent secondary infections, both pyodermas (bacterial skin infection) and Malassezia dermatitis (yeast dermatitis), are common clinical complications. Secondary infection will not only exacerbate the severity of the allergic pruritus, but it is also often non-responsive to common anti-pruritic treatments used for treatment of atopic dermatitis. Understanding and managing any secondary infection is a vital step to improving the treatment outcome for patients with allergic skin disease.
The most common bacteria associated with canine and feline pyodermas is Staphylococcus pseudintermedius.1,2 Less commonly, other Staphylococcus spp. including S. aureus, S. schleiferi, and other coagulase negative staphylococci can be associated with pyodermas.1 Malassezia pachydermatis is the most common species of yeast associated with Malassezia dermatitis. Diagnosing the causative agent of skin infections is important for directing appropriate antimicrobial therapy. The only way to differentiate between a bacterial pyoderma and Malassezia dermatitis is cytological evaluation.1,2,3
Cytology allows for the identification of various cutaneous microbes, inflammatory cells, and other cellular or neoplastic changes.2,4 Additionally, cytology can help quantify organisms and help gauge response to antimicrobial therapy.
Cytology is an invaluable part of the dermatologic database of tests and should be utilized throughout the workup and management of an allergic patient. If infection is undiagnosed prior to starting therapy for atopy, it can result in a perceived lack of response to anti-pruritic or anti-inflammatory therapy.
Additionally, if a previously well managed patient becomes less responsive to therapy, cytology is important to evaluate for breakthrough infection, which can skew or dampen the therapeutic response.
Another infectious roadblock in allergic patients is the development of a resistant secondary infection. Methicillin- and multi-drug resistant Staphylococcal pyodermas are becoming an increasingly frequent and challenging complication in allergic cases. Resistant pyodermas should be suspected in any cases in which there is lack of improvement with the appropriate dose and duration of an empirical antibiotic, a history of numerous previous courses of antibiotics, a rapid reoccurrence of lesions with cytological evidence of bacteria after complication of antibiotics, and/or a history of resistant pyodermas.1 If a resistant bacterial infection is suspected, an aerobic bacterial culture is imperative for directing further antibiotic therapy.
Finally, promoting judicious antibiotic therapy is crucial in allergic management and the prevention of development of resistant pyodermas. In addition to oral antibiotics, topical antimicrobial products, including sprays, shampoos, and foams, should be considered a critical part of all treatment plans. Topical therapy can be used to speed resolution of existing infections and as part of the maintenance therapy to reduce the risk of recurrent infections.
2) It’s not just environmental allergies
A second major roadblock in the management of allergic skin disease is overlooking non-environmental triggers of pruritus. These can be sole triggers or can be seen concurrently with atopy, including cutaneous adverse food reactions (CAFR), flea bite hypersensitivity (FBH), and other ectoparasites. Since atopy is diagnosed via exclusion of other allergic disease, a complete and thorough workup is recommended in all cases, but especially in those allergic cases unresponsive to empirical treatment.
Ectoparasitic diseases that can mimic the clinical signs of atopy are demodicosis, sarcoptic manage, and cheyletiellosis.1,4 Superficial and deep skin scrapings are strongly recommended as part of the initial dermatological exam to rule out parasitic triggers of pruritus and cutaneous inflammation. Additionally, a parasite trial treatment with consistent use of an isoxazoline flea and tick preventative can help rule out ectoparasites.2,4
In flea-endemic regions, FBH can be a primary trigger of pruritus or can dramatically exacerbate the pruritus in atopic dogs. Flea combing and evaluation for fleas on physical exam can be a great screening tool. However, consistent flea and tick prevention should be used for several months in all pruritic patients, even indoor only pets, to rule out a component of FBH in any suspected case of allergies.2,3,4
Finally, CAFR can be clinically identical to atopic dermatitis and can be seen alone or concurrently with environmental allergies. The presence of concurrent gastrointestinal signs, otitis externa, or anal sacculitis, a young or late age of onset of allergic disease, non-seasonal allergic signs, or lack of response to common anti-inflammatory and anti-pruritic therapies should increase the suspicion of a food allergy component.2,3,4 Diet elimination trials with prescription novel protein or hydrolyzed diets should be considered as the gold standard step to evaluate for cutaneous adverse food reactions.

3) There is no perfect treatment for atopic dermatitis
The main treatment options for atopic dermatitis can be broken down into two main treatment groups:
- Anti-pruritic and anti-inflammatory that focus on alleviation of clinical signs: glucocorticoids, cyclosporine, oclacitinib lokivetmab3
- Allergen-specific immunotherapy (ASIT) that focuses on desensitization with the goal of inducing tolerance to environmental allergens and possibly prevent the further development of allergic signs.2,5
When evaluating the response to a treatment plan for atopy, it is important to consider two major guideposts of success: reduction of pruritus and reduction of the frequency of secondary skin and ear infections. Unfortunately, there is no one-size-fits-all treatment for atopy, and the treatment plan must take into account the clinical presentation, tolerance and response to therapy in the patient, and limitations and goals of the owner.
When selecting the treatment option for an individual case, it is important to evaluate the unique allergic presentation. For example, while a predominantly pruritic patient with rare secondary infections might do best on the anti-pruritic focused lokivetmab, another pet with variable pruritus and recurrent otitis externa and pododermatitis may fail on lokivetmab but respond better to the broader anti-inflammatory control provided with cyclosporine.
Developing and finetuning an individualized plan, including systemic therapies and topicals, can be a daunting but rewarding part of the management of atopic dermatitis.
4) Owner compliance
Even with the best treatment plan in place, owner compliance and follow through with the therapeutic plan is vital for successful management of allergies in dogs and cats. In 2018, a review article looked at factors that affected owner compliance in the long-term treatment of allergic skin diseases. The authors found the chronic and severe nature of the disease, the expense associated with work up and treatment, and the need for lifelong therapy were major challenges for owners that often resulted in decreased compliance.3 Clear communication about the treatment options, costs and side effects associated with the recommended therapies, discussion of the expected timeline for improvement, and clear home care instructions and expectations of the owner’s role in the execution of the plan can help reduce owner frustration and improve adherence to the recommended therapeutic plan.3
Ultimately, there are many different treatment routes for allergic management, but it is important to look at these roadblocks as a detour back to the basics and not a dead end.
Rebecca Mount, DVM, DACVD, earned her Bachelor of Science in biology from the University of New Mexico in 2005, and her doctorate of veterinary medicine from Colorado State University College of Veterinary and Biomedical Sciences in 2009. Following graduation, Dr. Mount completed an internship in small animal medicine and surgery at Garden State Veterinary Specialist in New Jersey. She began her residency with Dermatology for Animals in 2010, and became a diplomate of the American College of Veterinary Dermatology
in 2014.
References
- Hillier, A., Lloyd, DH., Weese, JS., Blondeau, JM., et al. Guidelines for the diagnosis and antimicrobial therapy of canine superficial bacterial folliculitis (Anitmicrobial Guidelines Working Group of the International Society for Companion Animal Infectious Diseases. Veterinary Dermatology. 2014;25: 163-e43
- Miller, WH., Campbell, KL., Griffin, CE. Mueller and Kirk’s Small Animal Dermatology 7th edition (various pages). St. Louis, Missouri: Elsevier.
- Gedon, NKY., Mueller, RS. Atopica dermatitis in cats and dogs: a difficult disease for animals and owners. Clin Trasl Allergy. 2018;8: 41-53.
- Hensel, P., Santoro, D., Favrot, C., Hill, P., et al. Canine atopic dermatitis: detailed guidelines for diagnosis and allergen identification. BMC Veterinary Record. 2015;11:196-209.
- Griffin, CE., Hillier, A. The ACVD task force on canine atopic dermatitis (XXIV): allergen specific immunotherapy. Veterinary Immunology and Immunopathology. 2001;81:363-383.