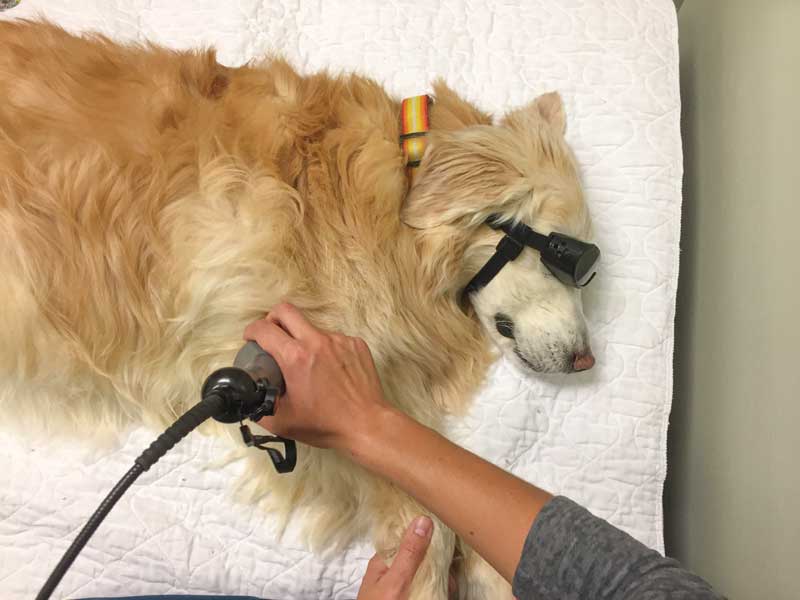
During my rehabilitation training well over a decade ago, I was taught how to use several devices to aid in treating my patients, one of those tools was a laser.
At the time, we were encouraged to purchase and use a class IIIb laser, which I did. Anecdotal evidence was presented showing a minimal difference between the IIIb and class IV devices. On top of that, it was suggested class IV devices were dangerous, with a real risk of setting my patients on fire!
I still remember the day my IIIb laser was shipped to me. I was excited to have another modality to treat my patients in pain. The learning curve was tedious at best, there was no software to help me determine dosing. Instead, I had to use the book that came with the laser and calculate all the factors and times to treat different areas of my patients. I forged ahead and used it on practically every patient I thought would benefit from this new therapy.
After about a month, I was seeing little to no benefit from the use of my IIIb. On top of that, I was doing literature searches on dosing, and it seemed most deep tissue (i.e. musculoskeletal) conditions required dosing in the range of 8-20 Joules/cm2. This new dosing increased my treatment time, in some cases, to 45 minutes or more. Due to a combination of lack of results and the poor time management of trying to treat my cases, I used the laser less and less. Eventually, one of my LVTs just put it away in a cabinet as it was “taking up space and gathering dust.”
A few years later, my good friend and colleague, Janice Huntingford, DVM, DACVSMR, was observing in my practice prior to being boarded in sports medicine and rehab at the time. Dr. Huntingford asked why I was not using a laser, and after several minutes of searching for it, I pulled out my IIIb laser and told her I was never convinced it was giving me the results I wanted, or even if I did see the result, it was not cost-effective due to the time it took to treat a patient. She convinced me I needed an upgrade and introduced me to my first class IV laser.
Learning to use my new laser took about 20 minutes. Most of the time was spent learning to use the software for calculating doses based on species, patient size and body condition, hair and skin color, and condition and area to be treated.
Once I understood the software and the adjustments in dose being made for the above-mentioned patient characteristics, setting up a new patient for treatment took less than a minute of my time. There were no complex calculations and double checking my work, everything seemed appropriate for the patients and conditions we were treating.
I had spoken to the manufacturing team and understood what the dosing protocols were based on (these are individual to each laser manufacturer so verifying is a must). The rest of the training was about how to use the laser itself and technique of treatment and treatment head selection to ensure optimal dosing and avoid any overheating of tissue.
Yes, the class IV produces more heat than the IIIb, but contrary to what I was taught, when properly addressed with different treatment technique, there was no danger of setting my patient on fire!
Dosing matters
The high power of my new laser has opened the door to new treatment possibilities. Suddenly, in just a few minutes, I am able to enter a new patient and treat them in the exam room with the owner present.
Conditions, such as ear infections, impacted anal glands, and hot spots take little time, and the treatment is usually administered by one of my LVTs, freeing me up to see my next patient.
Post-operatively, surgical incisions could be treated with the anesthesia off while the patient woke up from the anesthesia; something that was impossible to do with my old IIIb.
More importantly, with current research1 showing it is both energy density (J/cm2) and power density (W/cm2) that are critical to achieving success for deep tissue conditions and especially for chronic painful conditions, the higher power of my class IV device enables not only the treatment time efficiency, but also the saturation of light to deeper tissues that is not possible with lower irradiance devices.
Further, I could understand why some colleagues reported varying results with the modality as a whole (regardless of the class of laser they were using), with laser manufacturers being responsible for determining the dosing for each of their own protocols—the “hip arthritis” protocol from one device to another might vary wildly in its dosing.
Developing a partnership with a manufacturer that understands dosing and bases their protocols on current evidence is critical to clinical success.

Useful applications for photobiomodulation therapy
Pain. A huge part of my practice is pain management. A lot of my patients with chronic osteoarthritis cannot take NSAIDs, the “gold standard” for treating OA, for various reasons: kidney or liver disease, and prior gastrointestinal ulceration are the most common.
Therefore, I need to rely on physical modalities, and for me, that is usually laser therapy +/- acupuncture.
One advantage of photobiomodulation therapy (PBMT) is once I have the diagnosis and prepare a treatment protocol, my LVT can perform future therapies without my involvement. I only need to re-evaluate the patient from time to time. Laser therapy is especially important in the treatment of OA in cats that cannot take chronic NSAIDs and often will not tolerate needle placement during acupuncture.
PBMT also goes beyond simply taking care of the pain. There is an increase in the functionality of the tissues involved in the joint, the extracapsular areas around the joint, and the muscles associated with the movement of the joint.
For this reason, laser is a great therapeutic consideration at any stage of the disease and can complement classic and newer treatments, such as NSAIDS and bedinvetmab. How? Joint function is improved; reduced inflammation, which can reduce the rate of disease progression, help maintain and improve range-of-motion, which in turn improves joint lubrication through improved distribution of synovial fluid, which in turn allows for maintenance of muscle mass through improvement in the ability to use the leg and exercise it more.
Intervertebral disc disease (IVDD) and fibrocartilagenous embolism (FCE). IVDD is a painful condition that may or may not accompany paresis or paralysis. Sometimes it is so painful I cannot consider placing acupuncture needles as the dog will not tolerate them. PBMT fills this gap nicely, especially in the case of cervical disc issues, which seem to be the most painful spot for a ruptured disc. Most of these animals have the start of pain relief after just one treatment. If IVDD or FCE causes paresis or paralysis, this therapy will hasten the dog’s recovery and return to reasonable, if not normal, function.
Infections. Ear infections, anal sacculitis, acute moist dermatitis, and superficial wounds when treated with PBMT will heal much faster and with less pain than those dogs that do not get such treatment. These are changes the pet owner can often visually appreciate immediately after treatment.
Respiratory diseases. Asthma, bronchitis, and pneumonia all respond well to PBMT. It reduces inflammation, decreases airway spasm, and improves the exchange of air in the lungs, making the animal much more comfortable.
Chronic pulmonary fibrosis, or Westie lung disease responds better than those dogs that are only getting medication. One dog, in particular, that was on corticosteroids and bronchodilators, came to me in end-stage Westie lung, with a prognosis of only a few weeks left to live. We started with every-other-day treatments and eventually lengthened the interval to once every seven to 10 days. The dog went on to live for just short of two more years before succumbing to an unrelated cancer issue.

Conclusion
I really did go from skeptic to advocate of photobiomodulation therapy. Inadequate dosing, especially for deeper tissue conditions and chronic pain, can leave anyone with the impression that PBMT “doesn’t work” as a modality, when in reality it is no different than underdosing any other medication. If improvements are noted, they will be suboptimal at best and usually inconsistent. In this short article, I have only scratched the surface of what a laser can do.
I encourage everyone to consider the purchase of a laser, but with several caveats. Make sure it comes with software to help with treatment and dosage decisions, and the manufacturer you have partnered with has based their protocols on research (there is no standardization). Make sure that it is a true class IV laser, as there are some pretenders out there. Make sure the company will support you with continuing education, especially as new treatments and protocols become available.
Soon, your practice will be like mine, and you will need to buy a second laser just to handle all of your cases.
Michael Petty, DVM, is a graduate of the veterinary school at Michigan State University. As the owner of Arbor Pointe Veterinary Hospital and the Animal Pain Center in Canton, Mich., Dr. Petty has devoted his professional life to the care and well-being of animals, especially in the area of pain management. Petty is the past president of the International Veterinary Academy of Pain Management. A frequent speaker and consultant, he has published articles in veterinary journals and serves in an advisory capacity to several pharmaceutical companies on topics of pain management. Petty has been the investigator/veterinarian in 12 FDA pilot and pivotal studies for pain management products. He has lectured both nationally and internationally on pain management topics.
Reference
- Zein R, Selting W, Hamblin MR. Review of light parameters and photobiomodulation efficacy: dive into complexity. J Biomed Opt. 2018 Dec;23(12):1-17. doi: 10.1117/1.JBO.23.12.120901. PMID: 30550048; PMCID: PMC8355782.